Our health sector needs urgent healing
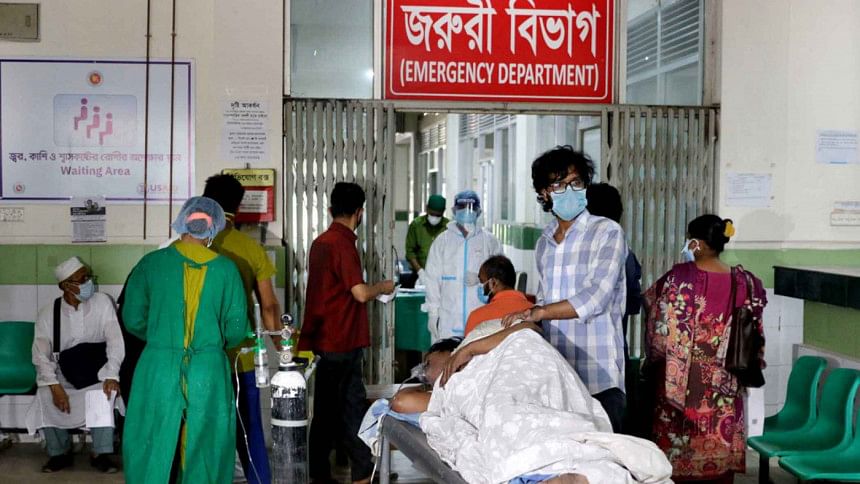
It seems the country's health directorate has finally been jolted out of its stupor. At a meeting last Wednesday, the Directorate General of Health Services (DGHS) came up with the decision of shutting down all unregistered health institutions within 72 hours. The countdown has thus begun.
After the meeting, the DGHS issued a circular, saying that the decision applies to all unregistered health institutions—those that are yet to apply for licences, those that have applied for licences but are operating without it, and those whose licences have expired and are yet to apply for a renewal. The regulatory authority even warned that operations of private hospitals, clinics and diagnostic centres will be stopped if the renewal application is not received within the specified deadline of 72 hours.
Needless to say, it's a very good initiative from the regulator. But one cannot be so sure of the measures to be taken since the DGHS has some precedents which are not encouraging. Such warnings were given in the past as well, with the last one being in July, 2020, when the DGHS set a deadline for private health facilities to obtain their licences by August 23 that year.
That move came following the revelation of a scandal in a private health institution, Regent Hospital, which was found to be providing fake Covid-19 certificates, although the DGHS entrusted the hospital with the responsibility of Covid-19 testing and treatment of patients. The law enforcement agencies conducted a drive at Regent Hospital and unearthed the gross irregularities there. It was even found that the hospital's licence had expired in 2014.
The revelation prompted the DGHS to issue the deadline of August 23, 2020 for private health facilities to obtain their registrations. At that time, health officials announced that legal action would be taken against those who did not complete the registration and licence renewal process by the deadline. Following the announcement, several thousand private hospitals, clinics, diagnostic centres and blood banks applied online to get their licences or for the renewal of licences with the DGHS. Any private healthcare service provider is bound to obtain a licence from the DGHS as per the Medical Practice and Private Clinics and Laboratories (Regulation) Ordinance, 1982.
But the process got stuck, with the owners of private hospitals and diagnostic centres saying that the conditions set by the government for registration and renewal of licences were difficult for many organisations to meet within such a short period of time. They appealed for a relaxation of some of the regulations. It should be mentioned that the government had started issuing licences online in 2018. There were allegations made by the owners' association that many private hospitals could not renew their licences due to limiting conditions, while the licences of many others were being renewed using bribes and without fulfilling any registration requirements. Unfortunately, we have seen a laid-back attitude of the regulators in addressing the problem, with health experts claiming that the DGHS only wakes up after incidents of gross irregularities surface at health facilities.
Last Wednesday's decision was no different. The DGHS awakened this time after the National Human Rights Commission asked it to take action against those responsible for the death of a pregnant woman and her unborn child during a Caesarean operation in Narail's Kalia upazila. Sheuli Begum, who was 25-years-old, and her unborn child, died on May 6 when an unregistered health official tried to complete the surgery at the local Hazi Khan Rowshon Ali Hospital and Clinic, which itself has no authorisation.
Although the DGHS has announced that it will take strict actions against errant health facilities, unfortunately, it does not know the exact number of such organisations. So, the question arises: Why does the health regulator not know the number of health organisations? This implies that the DGHS has no strong monitoring mechanism over the private organisations providing healthcare services. The lack of monitoring is also a reason why private hospitals can get away with overcharging patients.
According to the DGHS data compiled manually on November 8 last year, there are a total of 16,444 private hospitals, clinics and diagnostic centres across the country. Of those, 5,577 are private hospitals or clinics, 10,727 are diagnostic centres, and 140 are blood banks. Of all private hospitals, clinics and diagnostic centres, 10,892 have received their licences, out of the 16,132 that have applied via DGHS's online registration system.
There is no denying the fact that private hospitals and diagnostic centres have helped in supplementing the public healthcare sector in Bangladesh to a great extent over the last two decades. But it is not acceptable that countless health facilities are able to operate in the country without licences for years, while the DGHS only serves notices and warnings.
Herein lies the issue of poor governance in the healthcare sector. Despite making strides over the decades, the healthcare system of our country still lacks availability, equality and reliability. The pandemic exposed many gaps in our healthcare system, including poor governance and monitoring, corruption, and inadequate healthcare facilities.
The time has come for the DGHS to act and purge all corrupt elements that helped these dubious establishments to continue operations. For that, the government has to facilitate the DGHS with the required manpower to monitor health facilities across the country. This time, we would like to believe that the DGHS's decision would not remain ineffective like in previous cases. We would like to see an end to the nonchalant attitude of the authorities concerned in dealing with unauthorised health institutions. The directorate must stop the unregistered health facilities from playing around with the lives of innocent people.
Wasim Bin Habib is deputy planning editor at The Daily Star.

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 







Comments