Cancer care in Bangladesh: A tale of scarcity and negligence
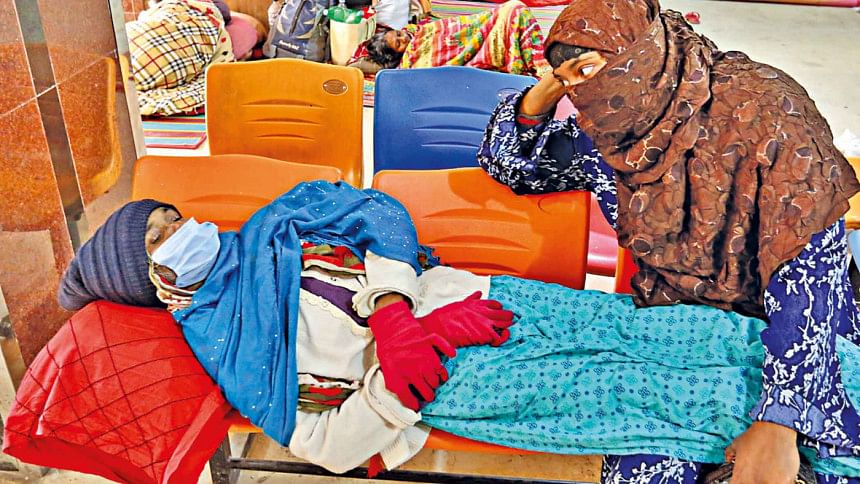
Due to overwhelming treatment costs, scarcity of trained professionals and unavailability of equipment, cancer care is still inaccessible to hundreds of thousands of cancer patients in Bangladesh.
Among 36 government medical college hospitals, which are the medical destinations for most of our country's low-income families, only 14 of them have oncology departments which are also undermanned and under-equipped.
Cancer patients in Bangladesh usually receive treatment in three ways: radiotherapy, chemotherapy and surgery. At present, only Chattogram, Rajshahi, Shahid Ziaur Rahman Medical College at Bogura and MAG Osmani Medical College at Sylhet have one unit of operational radiotherapy machine. Radiotherapy machines of Dhaka and Mymensingh Medical College Hospitals have been non-functional for years. There is not a single radiotherapy machine for the inhabitants of Khulna, Rangpur, and Barisal division.
According to Dr Qazi Mushtaq Hussain, professor of radiation oncology and director of National Institute of Cancer Research and Hospital (NICRH), Bangladesh needs at least 250 radiotherapy machines all over the country. At present, there are around 37 radiotherapy machines. However, the number fluctuates constantly due to frequent damage of these life-saving instruments.
Medical oncologists treat cancer by applying chemotherapy. In Bangladesh, facilities where chemotherapy is applied accurately are rare.
According to Professor Dr Zafor Md Masud, head of the oncology department of Bangladesh Medical College Hospital, "Safe handling of chemotherapy drugs is extremely important for accurate treatment and personal safety. These cytotoxic drugs must be prepared in biosafety cabinets equipped with high-efficiency particulate air (HEPA) filtration system to prevent contamination and inhalation. If the drugs get contaminated, efficacy of the treatment will be severely compromised." However, none of the government chemotherapy facilities and very few private clinics have this biosafety cabinet.
Moreover, there are only around 25 medical oncologists in the entire country. As a result, often radiation oncologists also treat patients with chemotherapy. Cancer patients who require surgery also have a hard time finding a reliable surgical oncologist.
According to Professor Dr AFM Anwar Hossain, one of the handful of trained surgical oncologists of Bangladesh, "There are around 30 surgical oncologists in the entire country. There is no surgical oncology department in the medical colleges which means almost all of them are based in Dhaka. Surgical oncology has only recently been introduced in oncology education in the country and currently provided only by NICRH."
As a result, most of the cancer surgeries are done by general surgeons who do not have oncological orientation.
"Cancer surgery is very complex in nature. Before conducting a surgery, a surgical oncologist must consult with radiation, medical and patho-oncologists about the type and nature of the tumour. Unfortunately, we cannot maintain this coordinated approach most of the time," adds Professor Dr AFM Anwar Hossain.
Bangladesh also lags behind in cancer diagnosis. Molecular tests such as Epidermal Growth Factor Receptor (EGFR) and BRCA are not available in Bangladesh which are essential for treating certain types of cancer.
Very few diagnostic centres conduct immunohistochemistry tests and PET-CT scans which are very expensive but essential for accurate diagnosis of cancer.
According to a 2020 report of International Agency for Research on Cancer (IARC), there are only 0.3 PET-CT scanners, 2.1 radiotherapy machines, 12.1 CT scanners, 4.6 MRI scanners, and 9.9 mammographs per 10,000 cancer patients in Bangladesh.
Due to a lack of these facilities, most of the cancer patients have to come to Dhaka for treatment and in Dhaka, NICRH is the apex government hospital where patients can go for comprehensive cancer treatment. Burdened with tens of thousands of patients, NICRH is far from providing quality treatment due to acute manpower and resource constraints.
According to Professor Dr Qazi Mushtaq Hussain, director of NICRH, "We have around 100 beds in chemotherapy day care section. However, we are providing chemotherapy to around 250 patients daily. Our doctors and nurses are working day and night without any extra allowances."
In December 2020, this hospital treated 46,883 patients with only 181 doctors. There are 45 vacant posts for doctors and 230 vacant posts for nurses, ward boys, and other support staff.

"We are suffering from manpower and equipment shortage. Many of our instruments are very old. We have asked for more manpower and modern equipment," adds the director of NICRH
According to experts, it is vital to monitor heart, liver, and kidney condition of cancer patients who receive chemotherapy or radiotherapy because cancer patients who receive chemo or radiotherapy often suffer from kidney, heart, and liver complications due to side effects of the cytotoxic drugs.
However, NICRH does not have any cardiology, hepatology, nephrology, or even palliative care departments.
Professor Dr Qazi Mushtaq Hussain said, "We do some primary monitoring but in case of any complication we have to send them to other specialised hospitals."
Patients have to go through a painful ordeal to receive treatment and care due to overcrowding and lack of essential services. At NICRH, hundreds of patients and their attendants were seen standing in long queues to buy tickets for treatment. Many patients who are too weak to stand were seen lying on the dirty floor as all the chairs were occupied.
Firoza Begum has been suffering from colorectal cancer for five years. Her daughter Shahana Akhter was holding her emaciated body and waiting for hours to buy a ticket.
Shahana said, "My mother is getting radiation therapy here. When we come to Dhaka for treatment, we have to rent a house because we have to wait for weeks to get an appointment. Every time we have to spend at least two to three months in Dhaka."
"Moreover, we have to conduct many tests and most of these tests are not available in this hospital. In the private clinics, cost of the tests is almost double. We have spent at least 30 lakh taka for my mother's treatment so far. We have sold all our properties except our home to bear the expenses," she added.
Cost of treatment in the private hospitals is even higher.
Aftab Ahmed was diagnosed with kidney cancer in 2019. His right kidney had to be removed surgically which cost 200,000 taka in a private clinic. Despite the surgery, the cancer spread to his abdominal wall and liver. Now, he has to take a drug called Everolimus which is highly expensive.
"A strip of 10 Everolimus tablets costs around 17,000 taka. I have to take one tablet a day. Besides, I have to conduct weekly tests of my liver and kidney which are also very expensive. The treatment cost is literally unbearable," said Aftab.
Professor Dr Zafor Md Masud said, "Every cancer patient has to go through medical check-up before and after each cycle of chemo or radiotherapy. Besides, if there are complications, the patients have to get admitted to hospitals which incur additional expenses. Expenditure can be reduced if we provide all sorts of treatment and tests in a single hospital so that patients do not have to move from one place to another."
"We need time and large-scale investments to develop such all-under-one-roof cancer hospitals. So, the best way to treat cancer now is to prevent it," he adds. However, according to experts, preventive cancer treatment in Bangladesh is in its rudimentary stage due to lack of population-based cancer registry (PBCR). According to IARC, an estimated 156,775 new cancer patients were diagnosed in 2020 and the number of cancer deaths so far is around 108,990.
Nevertheless, these numbers are based on the cancer prevalence in neighbouring countries because there is no source of cancer related data in Bangladesh.
According to Dr Habibullah Talukder Ruskin, a cancer epidemiologist and an associate professor of NICRH, "PBCR is a database which preserves detailed information about all cases of cancer that occur in a specific population. Even Nepal and Pakistan have their own PBCRs. India has 30 PBCRs which are centrally coordinated."
"Without PBCR, we actually cannot know how many patients develop cancer each year. We don't know how many patients die of cancer every year and what the most frequent types of cancer are among Bangladeshis. We don't have any data about the most common causes of cancer and district-wise prevalence. Without this basic information, how can we prepare for cancer prevention and treatment?" he states.
As a consequence, Bangladesh does not have any cancer control strategy and national cancer treatment protocol.
Surprisingly, Bangladeshi patients are treated according to the cancer protocol for US citizens called Evidence-Based Cancer Guidelines, developed by the US's National Comprehensive Cancer Network (NCCN) for their own citizens.
When asked why PBCR could not be developed in Bangladesh, director of NICRH said, "I don't know why it could not be developed. When I heard about developing PBCR I was a student. Now, I am on the verge of retirement. It is unfortunate that we still have not been able to develop it."
When asked what the government is doing to improve the country's dilapidated cancer care system, Professor Dr Qazi Mushtaq Hussain said, "The government is developing eight cancer centres in eight divisional medical colleges where there will be all the required departments, surgery facilities, and modern equipment. It will take some time but once this project is completed, cancer treatment will be decentralised and the situation will improve a lot. NICRH will also be transformed into a 500-bed hospital in the near future."

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 



Comments