Column by Mahfuz Anam: No Scope for Complacency
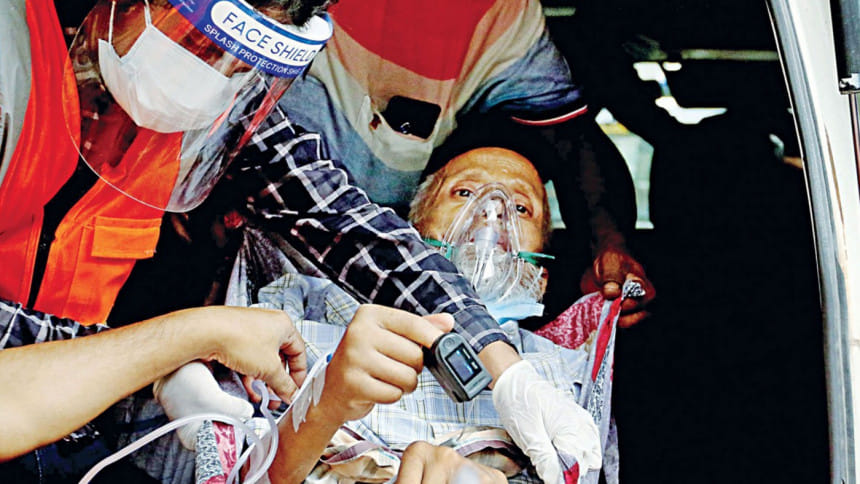
When Bangladesh was first hit by Covid-19 in March/April last year, we all thought that we would be seeing the end of it soon, at most by the year's end. One year down the line, we are rather worse off, not only for the lack of efficient management of the disease but also because of more deadly and virulent variants of the virus which are causing the second wave. This time around, we may be better prepared with more science-based knowledge but so is the virus—armed with various mutations—to penetrate our immune system. It is almost like a war of wits being waged between human ingenuity and the devilish disease, and the battle scene, for the time being, does not look good.
The lessons from India are many, with the principal one being not to get caught up in one's own words of self-congratulation—India does not have a monopoly on that score—and thus be lulled into a false sense of security which can lead to, as they say in sports, "taking the eye off the ball". Ankita Mukhopadhyay, in an article for Deutsche Welle (DW) on April 23, wrote that "despite having time to prepare, the Indian government focused on denial". While India held political rallies, election campaigns, and religious festivals, its daily infection rate went up from around 10,000 per day in February to above 300,000 per day in April. Such unpreparedness is most unbecoming for a country wanting to be a bigger player than a regional power.
The disaster that hit India - for which we express our deepest sympathy and sorrow and hope and wish that the people and government of India recovers from this nightmare at the earliest - has taken its neighbours by surprise. India has long been the natural destination for advanced healthcare treatment for many in South Asia. For that country to suddenly be in such a state of disarray, and to be unable to provide its own people with rudimentary facilities like oxygen, and for its hospitals—some of them quite renowned—to have to refuse treatment to critically ill patients, which literally amounted to pushing them to their death... all this seems quite surreal. The all-round collapse of the Indian health infrastructure has significantly taken the sheen off India's development narrative.
Keeping India aside, how prepared are we for the second wave? God forbid if that wave brings in either the UK or the Indian "double mutant" variant into play, then we really have a challenge in our hands. According to a report by The New York Times, "Doctors, the public and the media are citing anecdotal—but inconclusive—evidence to suggest that a homegrown variant called B.1.617 is driving the country's worsening outbreak. But researchers outside of India say the limited data so far suggests instead that a better-known variant, B.1.1.7., that walloped Britain late last year may be a more considerable factor."
Be it the UK or the Indian variant, it is proving to be highly virulent for the people, in many cases deteriorating into a critical stage within days if not hours of the infection. The danger is both clear and present.
So far, we have detected Brazilian, Nigerian, UK and South African variants in Bangladesh, of which the last is the most widespread. The presence of others is comparatively limited. The South African strain is known to be among the super-spreaders but is considered slightly less dangerous than the Indian variety. As is evident, so far we have been able to keep the second wave within manageable limits. But for how long, is an open question.
Our vaccine rollout, which began excellently, has suddenly stumbled due to the unexpected crisis in India. The Serum Institute of India has declined to supply us the contracted 30 million jabs after giving us only seven million at the urging of the Indian government, in spite of the fact that we have made advance payment. While India's domestic crisis is, of course, a factor to consider, yet there is a legal obligation to honour international contracts. We will expect the vaccine supply to be restored within the shortest time possible. Meanwhile, we have opened urgent negotiations with both China and Russia for a supply of their respective vaccines and we should credit our government for the quick expansion of vaccine sourcing, although it should be noted that we missed earlier opportunities when China had offered to conduct a third-phase trial of its vaccine—an offer we declined on cost-sharing grounds. A behind-the-scenes machination operated to sustain the monopoly of sourcing and prevent the government from expanding its vaccine options. Though late, we have now expanded our sourcing and given an emergency go-ahead to both the Chinese and the Russians.
Our attempts at ensuring public mask-wearing and social distancing have so far been a disaster. Basically unplanned, followed by half-hearted implementation and run by totally confusing and nonsensical directives, the lockdown as we have seen in Dhaka city so far did very little to mitigate the health concerns. Instead, it drastically affected the livelihood of the poor. First we had a lockdown, followed by a stricter version of it, and finally another stricter version where shopping malls are being allowed to open. What a farce! How can lockdown and mall opening go together?
The justification was obviously to appease the retail traders and shopkeepers. It is well-known that 60-70 percent of retail businesses in some items occur during the Eid festivals. However, it turned the lockdown into an effort devoid of any seriousness. From the looks of traffic jams, public gatherings and the general scepticism about the efficacy of mask wearing and social distancing, it is quite possible that a spike in infection rate with all its heart-rending consequences may occur anytime soon.
As preparations for the second wave, according to experts, we need to urgently attend to two things: increase the availability of oxygen, and expeditiously expand human resources in our health sector.
As for increasing our supply of oxygen, the Indian experience should leave no doubt in the minds of our policymakers as to how urgent and crucial a task this is. The current demand for medical oxygen is around 160 tons per day which we are able to meet, but only just. Any sudden spike in demand will instantly and drastically change the scene and a Delhi-like situation is not beyond the realm of possibility. Setting up new plants will take a year to become operational. So expanding the existing production capacity is the only practical option which, those who are familiar with the situation say, we easily can do. For that to happen, however, the government needs to urgently engage with the producers and help out with both credit and policy assistance so that they can increase their production capacities in the shortest time possible. Not creating the extra capacity for oxygen production on an emergency basis would amount to a criminal negligence of public responsibility.
The second and more complicated task is that of expanding our human resource in the health sector, by hiring more doctors, nurses and technicians and training them for the specialised task of Covid-19 treatment. In addition, we need a more scientific deployment plan for these frontline workers with time for adequate rest and relaxation embedded in their working hours. Treating Covid-19 patients continuously and seeing critical patients suffer and die frequently can create emotional and psychological strains resulting in trauma. Frontline health workers must be given adequate assistance in this regard. As of April 29, a total of 154 doctors and 23 nurses have died, and a total of 2,911 doctors and 2,567 nurses have been infected while saving the rest of us. In addition, 78.5 percent of doctors and 61.9 percent of nurses suffered from mental health related issues during the whole period of the pandemic, according to the Acta Scientific Neurology journal (See The Daily Star's lead story on Thursday).
While Dhaka and Chattogram are somewhat served, adequate and functional ICUs remain a crying need in the district headquarters and the smaller towns.
All in all, government efforts notwithstanding, we have been extraordinarily lucky as far as the pandemic is concerned. Some unknown factor has worked in our favour in keeping our infection and death rates comparatively low, although for the families that have lost their loved ones, the loss is incomparable.
To expect that we will be lucky for a second time is nothing short of foolish and irresponsible. We need to be far better prepared than in the past. The way our health ministry functioned in the last one year—being able to spend only 20 percent of its allocated budget for the current financial year—clearly shows that drastic changes are needed in the health sector both in terms of personnel and mindset. A shocking reality about the mindset is exemplified by the fact that not a single taka out of the Tk 100 crore allocation to the health ministry for research on the Covid situation was spent. The reason given is that the officials could not agree on a research methodology. Why do the officials need to meddle here? Give it to the professional researchers and they will determine the methodology. But, of course, our all-knowing bureaucracy could not let some academic tell them how to do research.
For God's sake, whatever else we do, let us not fall into that dangerous trap of complacency that we are "prepared" to handle a sudden worsening of our Covid-19 situation. We are NOT. Let us face that fact and work accordingly. The sad truth is, when governments make mistakes, only the poor and the destitute suffer. Others suffer too but not in the same devastating way. The rich always find a way out. Hence governments, beholden to the rich, do not mend their ways.
Mahfuz Anam is Editor and Publisher, The Daily Star.

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 




Comments