Everything you need to know about the new scourge of ‘black fungus’ amid the Covid-19 risks
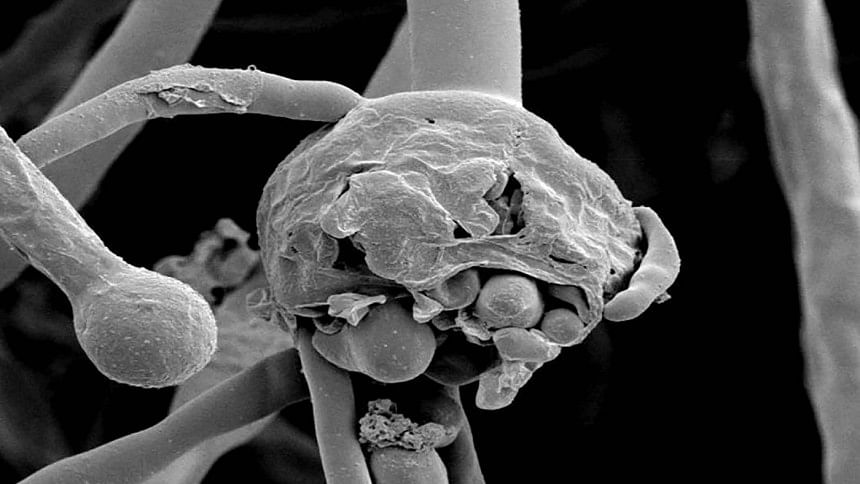
The world is already reeling under the Covid-19 threat, and now a new epidemic of 'black fungus' has surged in the neighbouring country, India. In Bangladesh, cases of black fungus have also been detected. Mucormycosis or popularly known as the black fungus is more prevalent among the Covid-19 patients or those who have recovered from the Covid-19 and have vulnerable immune systems due to the infection of the Covid-19 or have past records of diabetes. Here is what you need to know about this new healthcare scourge.
What is 'mucormycosis' or 'black fungus' infection?
According to the Centers for Disease Control and Prevention, mucormycosis is a rare fungal infection caused by a group of moulds known as mucormycetes. These fungi can be found in damp environments such as in soil or in decaying organic substances like compost, leaves or rotten wood. These fungal spores in the air can cause mucormycosis when they breathe in the spores of such moulds. It mainly affects the brain, the sinuses and the lungs after getting lodged in the nasal activity and in the adjoining tissues.
Who is at risk of this black fungus?
Black fungus is not harmful to most people, but it can be life-threatening for people with diabetes or HIV/AIDS or for those who have immunocompromising conditions like transplants and cancer. People with health problems or those who take medicines that weaken the immune system or lower the ability to fight against harmful germs and illness are also included in this vulnerable category. Amid this Covid-19 pandemic, patients who have been treated with steroids and other drugs can be at risk of this disease.
How can one get mucormycosis?
Mucormycosis is not contagious and so it does not spread from one person to another. It can happen any time after the infection of the Covid-19. The symptoms tend to appear either during the hospital stay or a couple of weeks later, after the discharge from the hospital or after the recovery. There are mainly three ways through which one can get infected with mucormycosis such as by inhaling these fungal spores or by consuming them through food or medicine or when these spores contaminate any wound. The most common way is the inhalation of the fungal spores. We actually breathe in many kinds of fungal spores every day. However, these do not cause any issue for us in case we have a healthy immune system.
Is there any treatment available?
According to the Centers for Disease Control and Prevention, the black fungus can be treated with antifungal medicines. If it is caught at the sinus stage, patients are more likely to recover than those with lung infections. In some cases, these drugs can have adverse effects on health such as sometimes it can lead to kidney issues, stroke or neurological dysfunction. Moreover, mucormycosis requires surgery in some cases, which can lead to the loss of an eye or the upper jaw. If you have any symptoms of black fungus, do not try to treat yourself at home or do not use any kind of drug without consulting a doctor. It can be life-threatening.
How to prevent mucormycosis?
Wear masks while going outside, especially while visiting dusty places. But do not use the same mask again and again. Maintenance of good hygiene is a must. One needs to maintain nasal and oral hygiene strictly. While gardening, do not touch the soil and plants with bare hands as these places abound with fungi. Use rubber gloves and masks while doing such jobs. Make sure that the surroundings of your home are free from dust and dampness. Try to keep the blood sugar level in control. It is more important if one has just recovered from the Covid-19. The use of steroids and other drugs needs to be limited. Do regular exercises and follow the hygiene rules all the time.
How risky is this infection?
Mucormycosis is rare, but a very lethal infection. Sadly, the mortality rate is too high in case of this infection. If the patients having such infection go untreated or treated late, the fatality rate is as high as 80%. Even if treated, the rate is still around 40-50%.
Symptoms of mucormycosis
There are different kinds of mucormycosis, but the one which is mainly noticeable amid the Covid-19 pandemic is- rhinocerebral (sinus and brain) mucormycosis. Initially, pain and redness around the nose or eyes, shortness of breath, fever, headache, coughing, and vomits with blood can be observed. Other common symptoms are:
Nasal blockage or congestion, bleeding and discharge from the nose;
Blackish discolouration on the nasal bridge or upper side of the mouth;
Blurred vision or double vision with pain, drooping of the eyelids;
Chest pain, limb weakness, seizures;
One-sided facial swelling, numbness, pain on the cheekbone;
Loosening of jaw movement, toothache;
Skin lesions, necrosis and thrombosis.
If anyone notices all or some of these symptoms, one should immediately consult with a doctor.

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 



Comments