<i>Treating poor patients: An ethical dilemma</i>
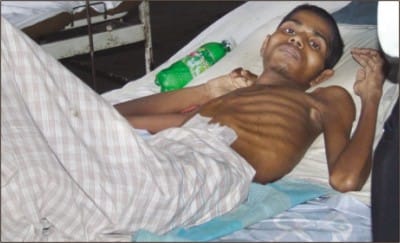
Farid Miah (not a real name), a 25 year old poor young man was recently admitted in Bangabandhu Sheikh Mujib Medical University (BSMMU) through outpatient clinic with the complaints of fever and extreme weakness. His X-ray chest was suggestive of a mass lesion at his chest. A possibility of Lymphoma, a kind of cancer was predicted.
However, in order to be certain about the proposed diagnosis, we needed a CT scan and a biopsy from the lesion. Performing a CT scan and biopsy are quite expensive and when added to actual treatment cost, the patient's family was in no way capable of paying for these expensive diagnostic procedures.
When doctors informed the family members that probably the patient had been suffering from a serious disease which needed expensive treatment. They faced the grim option of buying the diagnosis with treatment. They took the painful choice and requested us to treat his fever only so that they could take the patient back home at an outskirt village in Faridpur. They leave the cure of bigger disease to the mercy of God.
The case of Farid Miah is not unique in Bangladesh. Doctors have to deal with patients like Farid Miah very frequently. Obviously our public healthcare system does not have enough resources to provide the poor patients with expensive tests and medication.
In this sort of cases, many Bangladeshi doctors are tempted to start treatment assuming that the patient is suffering from the most common type of Lymphoma. Because, treatment of the most common type of Lymphoma is relatively inexpensive. Here comes the ethical dilemma of treating patients as per the medical guideline versus treating poor patients as a separate category in a way that is not taught conventionally. Thousands of cases like Farid Miah's force us to contemplate about developing and teaching new ethics and even developing new laws for providing appropriate care to poor patients.
Although doctors learn standard practice at medical institutes, in real life they constantly face dilemmas of standard patients vs poor patients. In many cases a doctor would decide to start treating a patient without all diagnostic procedures completed.
Many times newspapers carry stories of wrong diagnoses and the doctors are squarely blamed. While, not denying the case that sometimes mistakes are made by our doctors for many reasons including incompetence and negligence, it should be considered that most of our patients are poor and many a time running the full battery of recommended investigations before starting a treatment is beyond their means.
Again, if the doctor sticks to the literature and works within the constraints imposed by the existing laws, thousands of poor patients like Farid Miah would probably die without getting any treatment at all. Resolving this acute dilemma will not be helped by looking at the medical textbooks, which have originated in the western societies where poverty of the population is irrelevant in the arena of medical ethics.
On the contrary, poverty affects every aspects of healthcare in a country like ours. Therefore there is a serious need for developing ethical standard, norms and their legal counterparts for dealing with poor patients. There should be appropriate guidelines clearly stating what should be done when a patient can not afford all the necessary investigations. The law should also be clear on the liability of the doctor when s/he treats a poor patient based on inadequate investigations.
Developing such ethical guidelines is not an easy job. Doctors, philosophers and social scientists need to think, discuss and formulate new ethics that would fulfill the needs of our society. International bodies like WHO may help in initiating such discussion in national and international public domain.
The writer is a Professor, Clinical Hematology, Bangabandhu Sheikh Mujib Medical University (BSMMU), Dhaka. E-mail: [email protected]
The article is completely the opinion of the writer himself and does not necessarily reflect the views of Star Health.

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 




Comments