Fighting against Thalassaemia
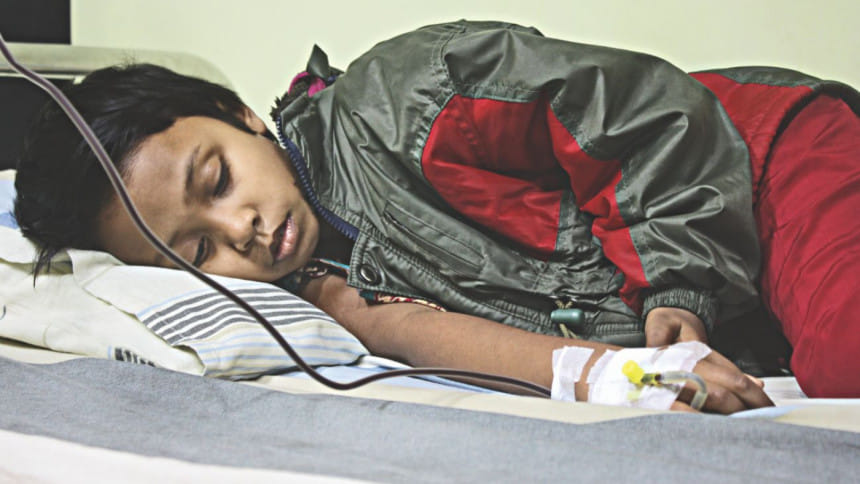
International thalassaemia day is observed all over the world on 8th May to create awareness of the disease among common public, discuss strategies to prevent the births of thalassaemic children and to also to pay homage to those who died.
This disease is mainly known to those families who discover that their child is suffering from thalassaemia when they go to a doctor with symptoms of anaemia, enlarged spleen and other complications and their happiness turns to confusion and shock when they learn that their child will have to be given regular transfusion and drugs through their whole life to keep them healthy.
Thalassaemia is a congenital haemolytic disorder where there is anaemia or low haemoglobin. It is the most common congenital disorder in Bangladesh as in many parts of the world. Blood contains iron and regular blood transfusion leads to accumulation of excess iron which is toxic and damages different organs of the body like heart and endocrine glands leading to organ failure and many other complications. This iron needs to be removed by chelating drugs (iron removing drugs) which has to be regularly taken and is expensive. Majority of our patients cannot afford adequate treatment.
A child is born with thalassaemia through their parents who are carriers of this disease. Carriers are healthy or may be mildly anaemic especially beta trait carriers and may be confused with iron deficiency. They are not aware of their status unless they do tests to know whether they are carrier of this disorder which unfortunately is rarely done as they are not aware of this disease and that it could have been prevented.
There are two common types of carriers in Bangladesh. Beta trait carrier where there is defect in synthesis of globin chain and HbE trait where there is structural defect. The frequency of beta trait carrier is 4.1% and HbE carrier is 6.1% which means that there 16 million carriers in our population with wide variation in distribution in different regions of Bangladesh.
In the coming years it is essential that serious efforts should be made to control thalassaemia problem and it has to be recognised as an important health issue. As the infant mortality rate and under five mortality is falling which is a big achievement of our government but more children are now coming to hospital with genetic disorders like thalassaemia. We do not want a population with sizeable numbers of genetic disorders.
Thalassaemia is a preventable disease. For a successful prevention support from all stakeholders is mandatory.
Creating awareness: Awareness about the disease can be made by holding seminars, workshops, and through the mass media.
Population screening: Population screening should be done to find out the carriers is an important pre-requisite for preventing the births of thalassaemic children. Screening can be done in college students, young couples before marriage or in early pregnancy.
Genetic counselling: As part of prevention of the births of thalassaemic patients, genetic counseling plays an important role especially to carriers and although the response may vary depending on the availability of prenatal diagnosis.
Prenatal diagnosis: Prenatal diagnosis allows a couple to abort a foetus (unborn baby) suffering from thalassaemia. It is usually done in the 10th to 13th week of pregnancy. The procedure has become relatively simple. Some countries like Iran, Saudi Arabia, Palestinian Territories, Greece and Cyprus have laws in place making premarital screening for haemoglobinopathies mandatory for all couples before they are given approval to get married. The choice is with the couple to abort an affected foetus.
The government should pay attention for prevention, care and management of thalassaemic patients. Every major hospital should have a thalassaemia centre, facilities for prenatal procedure and DNA labs to diagnose the status of the foetus and counseling for voluntary abortion of an affected foetus. The chelating drugs should be also should also be subsidised.
The writer is the President of Dhaka Shishu Hospital Thalassaemia Centre.
E-mail: [email protected]

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 




Comments