What if Kidneys Fail? Law stands in way of transplantation
At 23, her life should have been full of colours but instead it is as pale as it could get. This spring has brought her no joy at all.
For the last six months, both her kidneys have been failing to purify blood and balance body fluids, a function essential for survival. She undergoes dialysis, an artificial way to remove waste from blood.
The treatment is expensive; it has already cost her over Tk 2 lakh. A BBA student of a reputed university in Dhaka, she is now extremely worried about her future.
“I need dialysis three days a week. It's difficult for me to go to class and study,” she said.
In desperation, she wants to have a kidney transplant. And for this she needs a donor, who, according to the country's Human Organ Transplant Act, 1999, has to be from these relations: son, daughter, father, mother, brother, sister, paternal and maternal uncle and aunt, husband and wife.
Her cousin (daughter of her maternal aunt) wants to donate one of her kidneys, knowing that one is enough for a person. But the law does not allow cousins to be donors.
So she has decided to go to India, where non-relatives can donate kidneys, and sought financial help via newspapers as her family cannot afford Tk 20 lakh she will need there for a kidney transplant.
In Bangladesh, the cost is only Tk 3 lakh.
“Had my cousin been allowed to donate, I would not have to worry about money,” she said.
Life has become tough also for another kidney patient, a 33-year-old schoolteacher in Manikganj. She has already spent Tk 5 lakh in the last two years for treatment and dialysis.
Her friends are mobilising a fund of Tk 30 lakh for her kidney transplant in India. Her family is looking for a donor, failing to have one among the specified relatives.
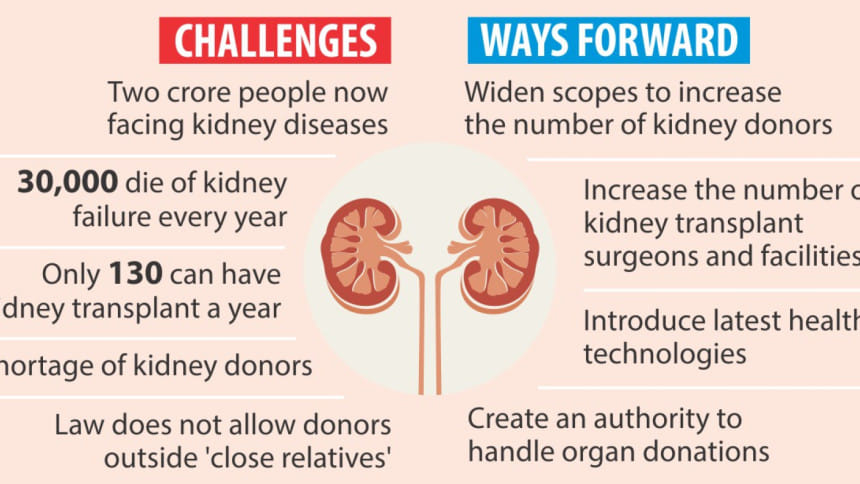
There are some 2 crore kidney patients in the country.
Every year, some 30,000 people die in Bangladesh failing to have kidney transplants or dialysis and some 40,000 become end-stage kidney patients.
“Lives of at least 20,000 could have been saved had their kidneys been transplanted,” said Kidney Foundation President Prof Harun Ur Rashid.
Tragically, only some 130 can have their kidneys transplanted here per year, he said. On the other hand, different hospitals in Kolkata alone transplanted kidneys of 140 Bangladeshis in 2016.
Many have kidney transplants in other places of India or in Pakistan, Sri Lanka, Thailand and Singapore. There are, however, allegations that many well-off patients having kidney transplants abroad fake documents to prove the donors are their close relatives.
Rabindranath Tagore International Institute of Cardiac Sciences (RTIICS) in a recent letter requested the Bangladesh Deputy High Commission in Kolkata to be watchful in issuing no objection certificate (NOC).
No Bangladeshi can undergo a kidney transplant in India without an NOC, which is meant to prove the donor and the recipient are close relatives, and the donation is not violating the 1999 act.
Though India allows non-relatives to donate kidneys, it follows the law of Bangladesh in cases of Bangladeshi patients.
RTIICS, a reputed hospital in West Bengal, transplanted kidneys of 111 Bangladeshis in 2016, 81 in 2015 and 41 in 2014, reports our correspondent Subrata Acharya from Kolkata.
Experts say while there is a shortage of kidney donors at home, the high cost of dialysis makes it impossible for most patients to continue the procedure.
Besides, there is a shortage of kidney surgeons and a lack of initiatives to increase the number of kidney donors within the existing legal framework that allows using kidneys of brain-dead persons.
Brain death is the complete and irreversible loss of brain function, which may be caused by accidents, stroke and primary brain tumour. In such conditions, their organs including kidney can be taken out and given to those needing it.
Law permits such transplants upon written consent from the brain dead person's appropriate relative, but no hospital has taken any initiative to make it happen.
A survey by the Kidney Foundation in 2007-08 found relatives of 25 percent of around 300 brain-dead persons would give consent if approached. The BSMMU and DMCH were picked for the survey.
The percentage can be higher with proper motivation, said Prof Harun.
Experts say the lack of latest health technologies is another obstacle to kidney transplant in Bangladesh.
Founder of Gonoshasthaya Kendra Dr Zafrullah Chowdhury, who himself undergoes kidney dialysis, said kidney disease has become no less than epidemic in the country where the shortage of donors is a big problem, which is causing organ trafficking silently.
On the other hand, the solvent patients are spending huge amounts abroad, Tk 25 lakh to Tk 1 crore.
Dr Zafrullah said any non-relative wishing to volunteer in donating organs should be allowed to do so. There is also scope for posthumous donation, he said.
For this to happen, he suggested setting up an authority to keep all the records of the donors and recipients and to handle the related issues under a law.
RESERVATIONS?
There are also reservations about allowing kidney donations by the non-relatives.
Dr SAM Golam Kibria, former professor of urology at the BSMMU, said the law allowing all to donate kidney is very likely to be abused in the country's current socio-economic context.
“There will be more and more organ trafficking and it may become a huge social and health crisis.”
Prof Harun too fears the same.
Dr Touhid Md Saiful Hossain, a transplant surgeon at the BSMMU, proposes inclusion of cousins, grandparents and grandchildren as kidney donors but not the non-relatives.
Dr Zafrullah, however, argues that kidney trade is already happening amid widespread kidney failure cases as the law limits kidney donation to the close relatives only.
“The government has to take stringent measures to stop any kind of organ trade. It should arrange incentives, including preferred healthcare facilities, for the donors,” he added.
Prof Harun argues that creating public awareness and introducing cadaver transplantation (taking organs from the dead) would significantly increase the number of kidney donors.
He said kidneys of those dying in road accidents are more suitable for transplantation. Even if half the road accident victims can be rushed immediately to the ICU, they will be a major source of kidneys.
“This requires a medical board at a hospital to declare brain death, emergency transport arrangement, intensive care unit facilities and a team of dedicated physicians.”
Every year, over 23,000 people are killed in road accidents and nearly 49,000 people die of stroke, according to an estimate. Many remain brain-dead after stroke or road accident but the exact figure is not available.
KIDNEY SWAP & NEW TECHNOLOGY
Experts say swap of kidneys is a good idea. For example, there are two couples -- Hasan-Amena and Jahurul-Khadiza. Hasan and Jahurul need kidneys and their blood groups don't match with their spouses'. But Amena's blood group matches with Jahurul's and Khadiza's with Hasan's. In such cases, Amena can donate kidney to Jahurul and Khadiza to Hasan.
“This is practised in many countries. We too can easily do it,” said Prof Harun.
Sometimes a close relative cannot be a donor just because the blood groups are not matching. But new technologies have made transplantation possible even if blood groups do not match but 25 to 50 percent tissue matches.
Such technologies are widely used in the US, Europe and Japan, and on a small scale in India. “We can introduce the new technology to increase the number of donors among the blood relatives.”
Prof Harun said there are some 20 kidney surgeons in Bangladesh working in only two public and seven private hospitals, which is quite low compared to the need.
Similarly, he added, there is also shortage of trained nephrologists, anaesthesiologists, nurses as well as the shortage of ICU and operation theatres for kidney transplant.
Dr Touhid said there should be incentives for both -- those involved in transplantation as well as the donors -- to promote the organ donation culture.
Prof Abul Kalam Azad, director general of the Directorate General of Health Services, admitted shortages of facilities and physicians, but said facilities would be expanded under a scheme for 2017-2021.
He said people have kidney transplants abroad for various reasons that may include their confidence in foreign healthcare system. Doctors in Bangladesh are very cautious about transplantation since the widespread media coverage of kidney trade in Joypurhat in 2011.
Regarding the law, he said it was the doctors who suggested many contents of the act of 1999. If the kidney specialists come up with new suggestions, the authorities will surely consider those.
“It is now more important than ever to establish the culture of organ donation to save lives,” Prof Kalam added.

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 



Comments