Five decades of growth in the healthcare system
In the last five decades, the health conditions of people in Bangladesh have improved due to the growth of our healthcare service sector. Our average life expectancy has grown from only 52 years in the 70s to the current 72 years. This has been accompanied by a reduction in infant and maternal mortality rates, growing access to healthcare and education, and progress in various social indicators. In 1990, 534 women used to die among one lakh pregnant women, which has come down to 173 in 2016. The infant mortality rate was 9.4 percent in 1981, which has come down to 1.9 percent in 2019. The Extended Immunisation Programme (Penta V) has been developed to fight various infectious diseases such as diphtheria, polio, whooping cough, hepatitis B, rubella and, above all, the BCG vaccine is now given six weeks after birth. Many hospitals in rural or semi-urban areas are working with local women to create awareness on maternal health and nutrition, family planning, prenatal maternal healthcare, etc. Other healthcare organisations and NGOs are also playing a significant role in raising awareness about primary healthcare and nutrition.
While communities working together in this way for their wellbeing is a sign of hope, there is a need to specifically look at the growth of the rural health system over the last five decades. At present, one-third (36.6 percent) of the 170 million people in Bangladesh live in cities, meaning that most of the country's population are still living in rural areas. But the major modernisation of the country's healthcare management has been city-centric. As a result, people are rushing to metropolitan areas for treatment and the city's hospitals are struggling to cope. The urban middle class are also travelling to neighbouring countries for better health treatment. According to the Center for Research and Information (CRI), there are around 600 government hospitals in Bangladesh at present, of which 482 primary service hospitals are upazila based. There are about 75 secondary hospitals in the districts and 15 hospitals where specialised medical services are provided. In addition, more than 15,000 community clinics and satellite clinics have been officially established for primary and child and maternal healthcare.
Despite having so many healthcare centres, community clinics and satellite clinics, why are people from rural areas rushing to big cities like Dhaka or Chattogram for medical treatment? According to government information, the number of public and private hospital beds in Bangladesh is about 1.5 lakh, and the number of private hospitals is almost double that of government hospitals. According to this calculation, the number of beds allocated for every 1000 patients in Bangladesh is less than one (only 0.87), whereas the World Health Organization (WHO) recommends a minimum of three beds per 1,000 patients for ensuring access to healthcare. In other words, there is no allocation of hospital beds for two-thirds of the patients in Bangladesh at present, despite the existence of a network of clinics for primary healthcare.
According to the World Bank, there is also less than one doctor for every 1,000 patient in Bangladesh (0.6), whereas the WHO recommends one doctor for every 1,000 patient. The proportion of doctors and nurses in Bangladesh is also very skewed—while there should be at least three nurses per doctor, there is currently less than one. In other words, the number of nurses is alarmingly low at present. Over the last five decades, there has been a significant lack of focus on the importance of the nursing profession for the healthcare sector, although finally in 2016, the government upgraded the nursing profession to second class and established several nursing colleges. However, the quality of education in most nursing colleges needs improvement.
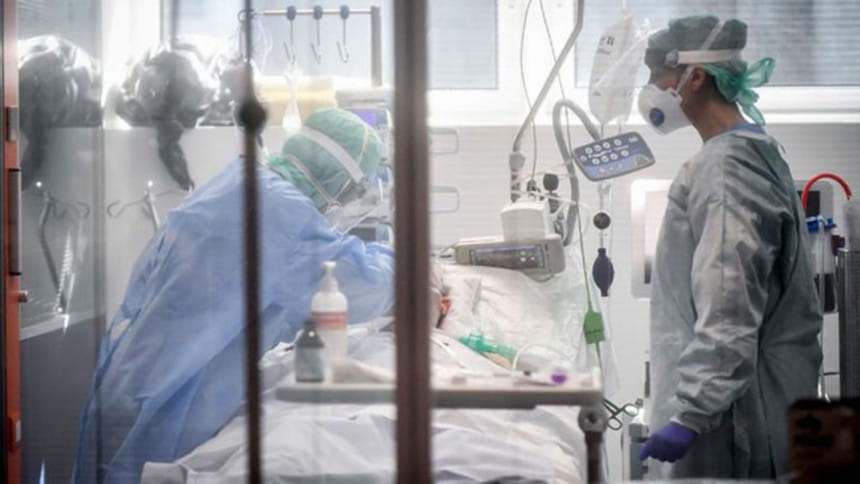
Intensive care unit (ICU) beds in the country is something else in which we are lagging far behind; there are currently not more than 1,200—of which 450 are in government hospitals and 750 in private ones—less than one per 100,000 patients. The number of high quality multi-disciplinary tertiary care hospitals is also negligible and most of these hospitals are in Dhaka. On top of that, patient pressure on specialist physicians is increasing due to the absence of a system of referrals in healthcare management. If this were properly implemented, patients at the primary and secondary level could get treatment from general practitioners so that specialist doctors could focus on the treatment of critical patients.
And it is not just ICUs—many district sadar hospitals lack CCU facilities and even elevators. There is often a shortage in power supply, and even if there is a generator, the allocation of fuel oil is not enough to run it properly. These problems are more evident at the upazila level. In some cases, the lists of medicine stored at the hospital are not drawn up or updated regularly. Although there are medicine counters in many upazila health complexes, there is often an inadequate supply of medicine, irregular supply etc. Most of these hospitals lack the necessary medical equipment, especially digital X-rays, CT scan, ultrasonogram and echo-cardiac machines, microscopes, etc. A majority of hospitals do not have operational ambulances.
At present Bangladesh ranks 88th in the latest rankings released by the WHO on the quality of healthcare around the world. Among the SAARC countries, only Sri Lanka is ranked 76th above Bangladesh. India is 112th, Pakistan is 122nd and Nepal is 150th. According to this ranking, the health system of Bangladesh appears to be better than that of India; yet Bangladeshi patients spend about USD two billion a year seeking treatment in India. We need to really get to the root of this issue.
Currently, Bangladesh is lagging behind other countries in health spending. Bangladesh spends 2.3 percent of GDP on the public health sector, whereas Nepal spends 5.6 percent, Sri Lanka 3.8 percent and India 3.8 percent. Developed nations like the UK tend to spend around 10 percent of GDP on healthcare. In Bangladesh, 65 percent of the allocation is spent on salaries and allowances, while the rest is meant to be on development. However, this allocation is clearly not fully utilised due to the lack of overall capacity of the health sector. It is not enough to increase the budget of the health sector—we must have good governance and proper healthcare management to ensure that the growth of the health sector is more uniform and equitable.
It is said that education is the backbone of the nation and health is the root of all happiness. Therefore, there is an urgent need to focus on improving the quality of healthcare in Bangladesh. A few recommendations can be made to bring the health sector under a robust structure—increase the number of beds and intensive care units by constructing quality secondary hospitals with individual incentives at the district and upazila levels; introduce patient referral system through digital connectivity in primary, secondary and tertiary hospitals; introduce health care insurance system and most importantly, prevent misuse of allocated budgets. We also need to encourage people to seek medical treatment in government hospitals, as well as set up public-private partnerships and encourage foreign investment in order to modernise these hospitals. Government hospitals can also outsource cleaning and support services in order to be better developed, and there is also a need to initiate health fairs and health camps in the villages and remote areas. Finally, we must aim for a better score on the Healthcare Index, which is an estimation of the overall quality of the healthcare system, healthcare professionals, equipment, staff, doctors, costs, etc. Currently, Taiwan is scored at 86.42, whereas Nepal is 57.44 and Bangladesh is 43.08.
Our health sector has a huge potential for good. However, we need skilled resources who will establish good governance with innovative strategies and build a vibrant health sector in the coming years.
Kishwar Imdad is CEO of a private healthcare company and AZM Saif is a communications professional.

 For all latest news, follow The Daily Star's Google News channel.
For all latest news, follow The Daily Star's Google News channel. 



Comments